Return To Running- Postnatal Guidelines
There are currently NO national/international guidelines that standardise practice and provide framework to support health professionals working with women who wish to return to running after having a baby. This is why the Return to running postnatal guidelines have been published by Grainne Donnelly, Emma Brockwell and Tom Goom. Since their guidelines have been published in March 2019 they have been used by many countries all over the world.
Athletics NI realise what a great opportunity it is for females to be able to access this research and for us to help you put them into practice.
Athletics NI have been working through the Return to Running Guidelines to pull out the most relevant information for those wanting to return to running - while remembering that ONCE A WOMAN IS POSTPARTUM THEY ARE ALWAYS POSTPARTUM and that you can start working on your Pelvic Health at any age. Your body takes time to heal after having a baby, it can take up to 15 months for everything to return to normal.
Looking after your pelvic health is also very relevant for females who are pre and post menopausal.
Athletics NI have put together the following guidelines based on the research by Tom Goom, Gráinne Donnelly and Emma Brockwell, in their 'Returning to Running Postnatal Guidelines for Medical, Health and Fitness Professionals Managing this Population'. You can read their full document here.
Although these articles are not tailored specifically to athletics, the information they provide is relevant to all sportswomen seeking to better understand and support their pelvic health.
Player welfare Pelvic floor article article for Camogie Ireland here
Pelvic Health Toolkit for England Rugby here
The below information is a condensed version of the 'Return to Running Guidelines' from March 2019.
Why do we run?
People run for a variety of reasons- to keep fit; to reach their distance goals; for their mental health; for those tempting endorphins; or simply for the social aspects the running community can bring. Whatever your reason, getting back into running after pregnancy can be a challenge and if you needed more motivation 'Running with a buggy increases your calorie burn by 20%’ https://www.telegraph.co.uk/health-fitness/body/on-your-marks-get-set-5-of-the-best-running-buggies/
What do we do?
At Athletics Northern Ireland, we host our twice-weekly in Belfast and once in Banbridge Buggy Club NI sessions for parents or guardians of young children who are keen to get active. We offer a range of running and core exercises, in a safe and friendly environment.
Below you will find information on assessing your pelvic health; examples to do before returning to running; objective measures for pelvic floor strength; examples of exercise progressions to do before returning to running and Tips for Running with a Buggy.
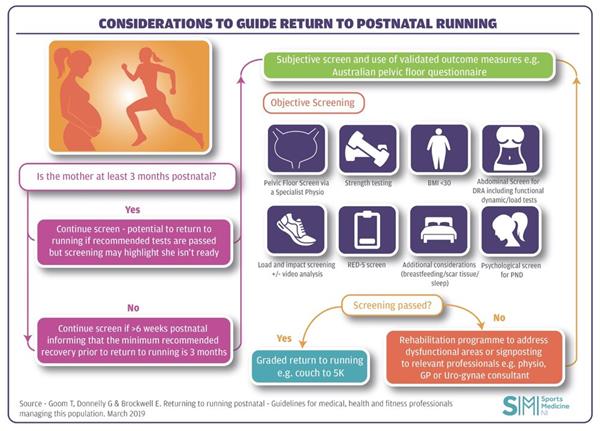
Assessment of Pelvic Health
Running is a high impact sport placing a lot of demand on your body. To be 'run ready' your body needs time to heal and regain its strength after having a baby.
Return to running is not advisable if any of the following subjective or objective issues are identified during screening.
Subjective symptoms: if any of these symptoms are experienced prior to or after attempting return to running then you should contact a pelvic health physiotherapist (page 12 of guidelines)
- Heaviness/ dragging in the pelvic area (can be associated with prolapse)
- Leaking urine or inability to control bowel movements
- Pendular abdomen or noticeable gap along the midline of your abdominal wall
- (this may indicated Diastasis Rectus Abdominis (DRA))
- Pelvic or lower back pain
- Ongoing or increased blood loss beyond 8 weeks postnatal that is not linked to your monthly cycle.
Objective measures for pelvic floor (page 14 of guidelines)
These tests are preformed by a health professional. The consensus of this guide is that running is less advisable if there is lower than Grade 3 Modified Oxford Manual Muscle Testing (MOMMT- Grade 3: able to contract your pelvic floor through full range against gravity) score during digital vaginal (Laycock and Jerwood 2001) or ano-rectal examination. Testing in both crook lying and functional positions, e.g. standing, is recommended to get a true indication of pelvic floor function and pelvic organ support.
If you have reduced pelvic floor muscle endurance, use the recommended guidelines below as a baseline for starting pelvic floor exercises:
- ✓ 10x fast reps
- ✓ 8-12 reps of 6-8 second maximum voluntary contraction
- ✓ 60 seconds submaximal 30-50% contraction
Here are a few cues to help you engage your pelvic floor, courtesy of White Circle

Additional factors for consideration (pages 18 – 23 on the guidelines)
The following factors must be taken into consideration as part of the postnatal evaluation
- Weight- Being overweight increases the load on your pelvic floor.
- Fitness- Encourage safe and appropriate, early postnatal fitness work.
- Breathing- Encourage a slow pace on initial return to running, such that would allow the individual to maintain a conversation.
- Psychological status- Screening for Post-natal depression (PND) is appropriate as part of assessment of readiness for Sport.
- Diastasis Rectus Abdominis (DRA)- the separation of the outer most abdominal muscles.
- Scar mobilisation- considerations of scar mobility and the need for scar mobilisation should be given regardless of mode of delivery.
- Breastfeeding- The World Health Organisation (WHO) advise women to breastfeed for at least the first 6 months postnatal and up to 2 years (WHO 2016). It is likely that women embarking on returning to running are still breastfeeding. it is recognised that breastfeeding prolongs the presence of a hormonally altered environment in the postnatal mother with lower levels of oestrogen and the possibility for slightly raised levels of relaxin to continue.
- Supportive clothing- Women may benefit from wearing a personally fitted sports bra that offers support rather than compression (McGhee et al. 2013) as this provides significantly increased breast and bra comfort. Sportswear and clothing aimed at supporting the pelvic floor and lumbopelvic area is gaining increased awareness and understanding for the benefits that they may have (Okayama et al. 2019).
- Sleep- Sleep is key for recovery from both physical and psychological stress and is frequently restricted in the postpartum period and beyond. Sleep deprivation in athletes is associated with increased injury risk (Milewiski et al. 2014), lower general health and increased stress. (Biggins et al. 2017)
- Relative Energy Deficiency in Sport (RED-S)- previously referred to as the Female Athlete Triad Syndrome it refers to impaired physiological functioning caused by relative energy deficiency including impairment of metabolic rate, menstrual function, bone health, immunity, protein synthesis and cardiovascular health (Mountjoy et al. 2014; 2015).
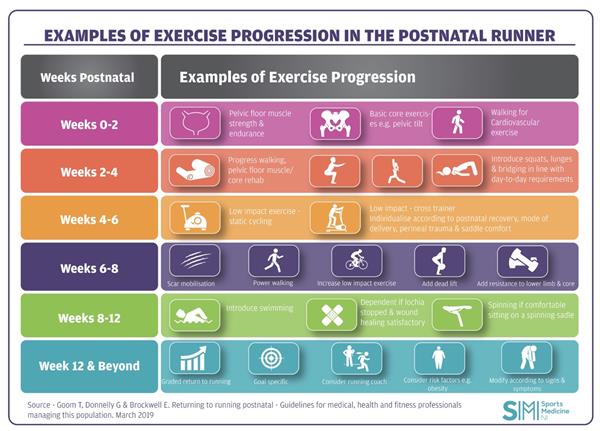
Example of exercise progression for the early postnatal period (0-3 months)
Week 0 to 2
- Pelvic floor muscle exercises (once catheter removed) targeting strength and endurance functions.
- Basic core exercises e.g. pelvic tilt, bent knee drop out, side lying abduction.
- Walking (for cardiovascular exercise).
Week 2 to 4
- Progress walking/pelvic floor muscle/core rehab.
- Consider introduction of squats, lunges and bridging, in line with the functional requirements of day-to-day life as a new mother.
Week 4 to 6
- Introduce low impact exercise e.g. static cycling or cross-trainer taking into account individual postnatal recovery, mode of delivery and perineal trauma. Recovery should be such that the new mother is comfortable sitting on a saddle.
Week 6 to 8
- scar mobilisation (for either c-section or perineal scar)
- power walking
- increased duration/intensity of low impact exercise
- deadlift techniques beginning at light weights no more than the weight of the baby in a car seat (15kg) with gradual load progression e.g. barbell only with no weight. This aims to strengthen and restore strategies for carrying out the normal everyday tasks required when caring for a newborn and/or older siblings.
- resistance work during core and lower limb rehab
Weeks 8 to 12
- Introduce swimming (if lochia has stopped and there are no issues with wound healing).
- Spinning (if comfortable sitting on a spinning saddle).